- A new study has found a decline in the number of people getting bariatric surgery for weight loss.
- The widespread availability of GLP-1 medications and weight management programs is likely contributing to this trend.
- Experts say that bariatric surgery has been shown to be an effective long-term strategy for weight loss.
- Bariatric surgery also has quick recovery times due to procedural advancements, such as laparoscopic techniques.
- Your doctor can help you decide whether weight loss surgery or weight loss drugs are best for you.
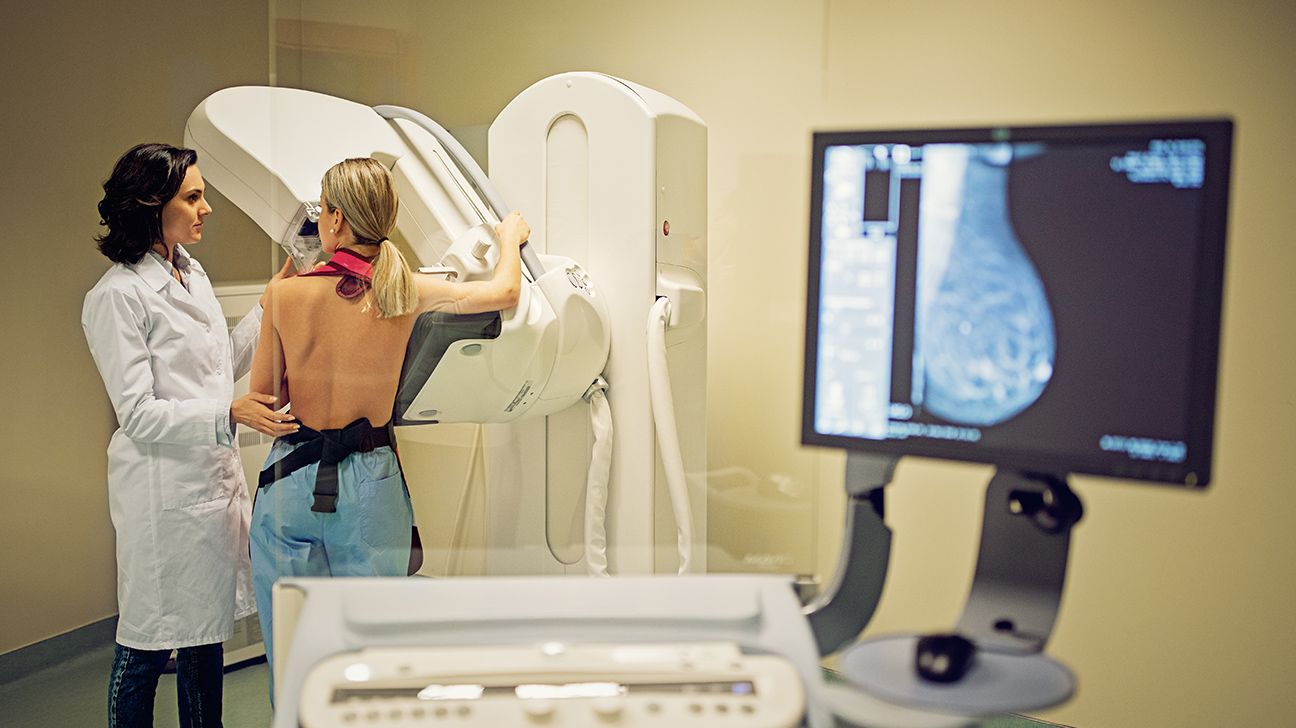
Until recently, bariatric surgery was considered a first-line treatment for weight loss.
The study’s authors aimed to understand how the types and numbers of bariatric surgeries have changed in response to the growing popularity of GLP-1 drugs and other weight loss treatments.
After examining data from 2020 to 2024, the researchers observed a decline in the number of bariatric surgeries performed across the United States.
The study highlights how patients and doctors are increasingly opting for surgery alternatives, reflecting evolving attitudes and options to treat obesity.
However, as noninvasive therapies advance, it’s important to track how these shifts affect surgical practices and patient choices.
To investigate these trends, the researchers analyzed a large national database called the ACS-MBSAQIP, which tracks bariatric surgeries performed in the United States.
They focused on surgeries performed from the beginning of 2020 through 2024, including both initial weight loss surgeries and follow-up revision or conversion procedures — procedures performed to modify or adjust earlier operations.
The data revealed that the overall number of bariatric surgeries reached its highest level in 2022, then declined in the following years. This drop reflects a growing preference for nonsurgical options among patients and healthcare professionals.
Alongside this reduction, the study found that the types of surgeries being performed have also shifted.
One key finding is a decrease in the frequency of sleeve gastrectomy, a common procedure in which a portion of the stomach is removed to reduce its size. While still the most popular surgery, its share of total procedures has steadily decreased since 2020.
In contrast, Roux-en-Y gastric bypass surgeries — which create a small stomach pouch and reroute the intestines — have become more common, particularly as conversion surgeries. Many people who initially had a sleeve gastrectomy later undergo a gastric bypass to further aid weight loss or address complications.
Additionally, the study noted an overall increase in other bariatric procedures, including sleeve gastrectomy, gastric bypass, and lap-band surgeries. This suggests that surgeons and patients are exploring a wider variety of surgical options tailored to individual needs.
By examining these trends, the study sheds light on how the field of weight loss treatment is evolving. It underscores the importance of ongoing research and adaptation in medical practice as new therapies emerge and patient preferences evolve.
John DeBarros, MD, Chief Medical Officer at Pivot Weight Loss Center, said he doesn’t necessarily feel this trend is either positive or negative for those seeking help with weight loss. DeBarros wasn’t involved in research.
“The honest answer would be it depends,” he told Healthline. “It depends on the reason why patients are making that choice.”
If they have researched their options and discussed their decision with a qualified surgeon before making their decision, and they still feel that a GLP-1 medication is best for them, that’s patient-centered care, according to DeBarros.
“What very much concerns me deeply, however, is when patients bypass surgery simply because GLP-1 feels easier or the less intimidating choice,” he said.
“I think the decline in bariatric surgery becomes a grave problem when patients with severe obesity, those with a BMI of 35+ with serious comorbidities, without understanding that surgery may be infinitely more effective for them,” said DeBarros.
Sergey Terushkin, MD, a bariatric surgeon with ThinEra, added that he thinks the conversation around GLP-1 medications has become too extreme on both sides. “Some people act like bariatric surgery is suddenly obsolete, other people dismiss the medications completely,” he told Healthline. “Neither is true.”
However, Terushkin, who was also not part of the study, acknowledged that GLP-1 drugs “have absolutely changed the field.”
“That’s a good thing,” he said. “Surgeons shouldn’t be angry that some patients are improving without an operation.”
With more weight loss treatments becoming available, it’s important to understand your options so you can make the best choices for yourself.
According to Terushkin, bariatric surgery is still the most effective treatment long term, based on years of data.
“Surgery is not just ‘making the stomach smaller,’” he explained. “It alters hunger hormones, metabolism, diabetes progression, sleep apnea, blood pressure, [and] mobility.”
Terushkin added that laparoscopic surgery, a type of procedure where a thin tube with a camera and a light on it is inserted through an incision in the abdomen, is not what many people expect. It allows most to recover quickly and go home soon after surgery.
“What concerns me most is when patients delay treatment for years waiting for a perfect answer that probably doesn’t exist,” said Terushkin. “I’ve done revision surgeries on patients who spent ten years bouncing between diets, supplements, medications, then came in with worsening diabetes and major health problems.”
Terushkin said that the best treatment really depends on the individual.
“Severity of obesity matters. Medical history matters. Whether someone can realistically stay on medication long term matters,” he said. “Sometimes medications are enough. Sometimes surgery is the better option. Sometimes they work very well together.
“The worst approach is treating obesity like there’s one universal answer for everybody,” he said.
While weight loss surgery has the most research supporting its long-term effectiveness, it’s also important to discuss your options with your doctor to determine what is best for you.