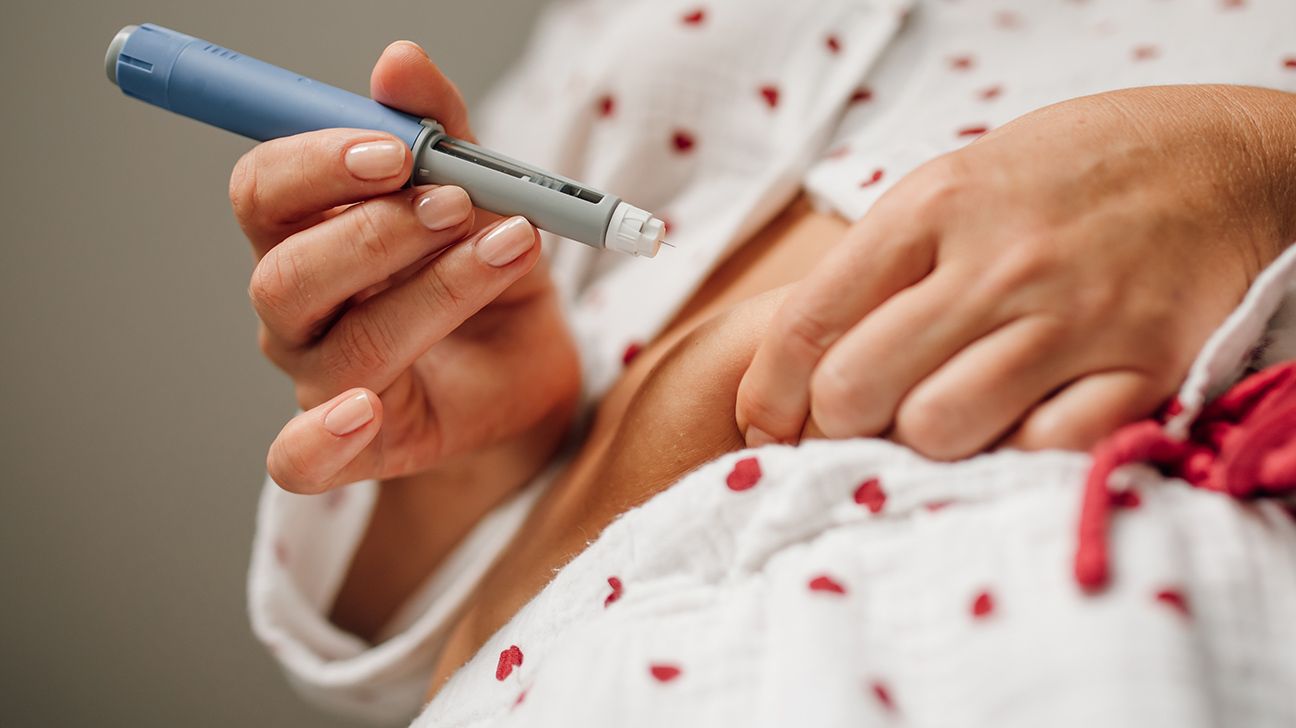
- A recent study found that GLP-1 drugs like Ozempic and Wegovy may significantly reduce blood pressure.
- The positive results were observed alongside weight loss and independently of it.
- The findings add to growing evidence to support the meaningful health benefits of GLP-1 drugs beyond weight loss.
Obesity and high blood pressure are closely related chronic health conditions that are of growing concern globally.
The two conditions have an interlinking web of causation, where obesity can play a significant role in the development and exacerbation of high blood pressure (hypertension).
A new meta-analysis shows that GLP-1 medications, such as Ozempic, Wegovy, and Mounjaro, can help significantly reduce blood pressure.
The findings indicate that the reduction in blood pressure was both weight-dependent and independent of weight loss.
The study, recently presented at the European Congress on Obesity in Istanbul, Turkey, from May 12–15, has not yet been published in a peer-reviewed journal.
“Given that obesity and hypertension frequently coexist and together substantially increase cardiovascular and kidney risk, these findings support obesity treatment as an important component of blood pressure management and cardiovascular risk reduction,” said lead researcher Marcel Muskiet, MD, PhD, an internist, endocrinologist, and vascular medicine specialist in the Department of Medicine at Leiden University Medical Center (LUMC) in the Netherlands.
“Our analyses suggest that the blood pressure benefits of GLP-1-based therapies are not exclusively driven by weight loss. While weight reduction appears to be the dominant mechanism, these agents may also exert direct renal, vascular, and neurohormonal effects that contribute independently to blood pressure lowering,” Muskiet told Healthline.
The researchers conducted a meta-analysis of phase 3 clinical trials. They were examining the relationship between weight loss and reduced blood pressure with GLP-1s and multi-hormone receptor modulators (MHRMs).
This analysis included 32 phase 3 trials that included 43,618 adults with overweight or obesity. The average age was 54, and the average body mass index (BMI) was 35.5. Around 50% of individuals were female, and 9.2% had type 2 diabetes.
Around 59% of participants were living with high blood pressure, and the average treatment period was 66 weeks. After placebo adjustments were taken into account, the average weight loss was around 10.9%. This was accompanied by a 5.2 mmHg reduction in systolic blood pressure.
The analysis showed that 77% of the variance in blood pressure could be explained by weight loss associated with GLP-1 drugs and MHRMs. This corresponded to a 0.34 mmHg reduction in systolic blood pressure for every 1% of weight loss.
“These findings showed an improvement in hypertension in direct correlation to the amount of weight loss,” said Mir Ali, MD, a bariatric surgeon, bariatric medicine specialist, and medical director of MemorialCare Surgical Weight Loss Center at Orange Coast Medical Center in Fountain Valley, CA. Ali wasn’t involved in the research.
“This reinforces the role that obesity plays in hypertension as well as many other health conditions,” Ali told Healthline.
The researchers noted that even without weight loss, GLP-1 drugs and MHRMs may help lower blood pressure. This may be due to their ability to relax blood vessels, improve kidney salt handling, and reduce stress signals.
“Though more research is definitely warranted to look at the mechanisms by which GLP-1 medications may work, I have seen some studies indicating that it may be a reduction in chronic inflammation,” said Ali. “Chronic inflammation can contribute to many health conditions, and obesity is a leading cause of chronic inflammation.”
Muskiet explained that the GLP-1 therapies may have various effects independent of weight loss. He said that potential mechanisms include:
- increased kidney sodium excretion
- improved endothelial and vascular function
- reduced arterial stiffness
- modulation of sympathetic nervous system activity
The researchers further noted that their meta-analysis had limitations and that more studies are needed.
“The main message is that obesity treatment and blood pressure management should increasingly be viewed as interconnected rather than separate therapeutic goals,” said Muskiet.
“Modern obesity pharmacotherapies are not simply weight-loss agents; they may become an important component of integrated cardiovascular risk reduction strategies in people living with overweight or obesity.”
GLP-1 medications were originally developed to help manage type 2 diabetes. They have also become popular tools for weight loss and weight management.
A growing body of evidence suggests that this class of medications offers other health benefits.
“There have been studies showing GLP-1 medications improving cardiovascular health, cognitive health, [and]
Recent research has also shown that GLP-1 drugs may be associated with improved breast cancer survival rates and reduced recurrence in people with obesity and related conditions.
Research examining the additional health benefits of GLP-1 drugs is ongoing.